“And so it was, whenever the spirit from God was upon Saul, that David would take a harp and play it with his hand. Then Saul would become refreshed and well, and the distressing spirit would depart from him.”
I Samuel 16:23 (NKJV)
Music universally touches the soul. There is abundant evidence of how effectively music calms, soothes, and relieves the frustration and anxiety of those loved ones among us who, because of neurology and/or biology, are unable to always fully verbalize their needs and responses to our desire to meet them.
We grew up in home filled with music. Although neither of my parents was a musician – and they had only a 33% success rate of their children becoming musicians – they loved music. They had an eclectic and surprising, at times, range of tastes and genres. So from our earliest memories, music became the a mainstay of our lives.
My mom was the musical adventurer in our family, embracing and exposing us kids to a rich landscape that remains for us even though Mom and Dad are gone. I think I was the inheritor of Mom’s legacy, though, because my musical journey has always looked and looks much like hers in its breadth and diversity.
I will never forget a little road trip that Mom and I took just after U2’s The Joshua Tree was released. I loved U2’s 1983 album, War, but had been disappointed with everything before and after that until the release of The Joshua Tree. I was playing it and Mom asked me to turn it up.
I turned it up loudly enough so that she could hear the music and the words – and handed her the liner notes so she could read the lyrics – and as she listened and read, she smiled and said “I like this. It reminds me of the music I heard growing up.”
As I thought about it, I realized she was right about the striking similarity in tone and content between The Joshua Tree and the Depression-era music she’d grown up with that juxtaposed the discouragement with the harsh reality of life then with the hope and optimism of faith and belief in God and I understood that we both appreciated the album for the same reasons in different time periods.
One of her favorite tracks was “In God’s Country:”
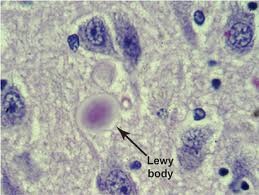
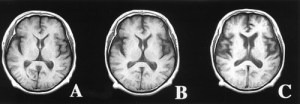
As Mom’s vascular dementia, Lewy Body dementia and Alzheimer’s Disease progressed, I turned back to music for her to calm her, to comfort her, and to bring back happier times and memories of her life. And, as Mom took her last journey out of this life, I also turned to the same music for the same reasons.
(Ironically, so far, it is really hard for me to listen to all of Mom’s music yet without a lot of sorrow except in small bits and pieces here and there where I don’t have the opportunity to linger over it and have the flood of memories of our life through the years come over me like a tsunami wave.)
With technology, building a customized musical library for our loved ones suffering from Alzheimer’s Disease and dementias have never been easier. I will list a few low-cost and free options for building these databases for playback at any time.
 Spotify has one of the largest musical databases around and is an excellent choice. An unlimited subscription is only $4.99 a month and provides unlimited play time with no commercials (the free version gives you 10 hours of playback a month with a lot of commercials). The “shuffle” feature works well with mixing the music up and making each playback unique.
Spotify has one of the largest musical databases around and is an excellent choice. An unlimited subscription is only $4.99 a month and provides unlimited play time with no commercials (the free version gives you 10 hours of playback a month with a lot of commercials). The “shuffle” feature works well with mixing the music up and making each playback unique.
While Mom was alive, I had the unlimited subscription. I created several playlists for her that we listened to a quite a bit during the last year of her life. A lot of times I’d play them softly during her naps, which became more frequent and lengthy during the year.
But when she was awake, we’d talk about the music and occasionally, we’d sing along if we both knew the words or I would sing to her and she’d smile watching and listening to me.
If you’d rather build your own musical database, the easiest way is to convert YouTube videos to MP3 files and download them to your computer (I’d suggest storing them in your Music folder in the respective folders you’ll need to create for different types of music or artists to keep them organized and easily accessible), where they can be played back with Windows Media Player.
The steps to do this are fairly simple:
- Copy the YouTube video link you want to convert to an MP3 file
- Go to listentoyoutube.com and paste the link

- Follow the directions for downloading the converted file
- Double-click on the file to play it in Windows Media Player
Once you’ve got Windows Media Player open, you can create playlists there and drag the MP3 files from your Music folders into each playlist. Then the next time you want to listen to a playlist, simply open Windows Media Player and click on the playlist. Windows Media Player also has a shuffle feature, which I would suggest using just to keep the order fresh and different each time a playlist is played.
So, if we haven’t already tried music as a comforting and soothing part of caring for our loved ones with Alzheimer’s Disease and dementias, then we need to implement it today. The benefits are not just to those we love because this is a wonderful way to connect and spend time together and intersperse some happy memories for us to carry with us when our loved ones are gone.