There are many kinds of dementia. In the next few posts, we’ll take a look at a few of them, along with Alzheimer’s Disease, which is a distinct neurological diagnosis from dementias.
Before we start, it is important to note that our loved ones can suffer from only Alzheimer’s Disease or only one kind of dementia. Or they may suffer from Alzheimer’s Disease and multiple kinds of dementia. That distinction is important to loving caregiving, which includes medical advocacy for our loved ones, because each brain disease is distinct, affects the brain differently, and has specific characteristics and symptoms and treatment.
I will admit here that one of my pet peeves while caring for my mom was hearing some people who have no real knowledge of these diseases lump everyone who suffers from them under Alzheimer’s Disease and giving advice on how to deal with that, not realizing the complexity of the situation posed by the presence of both dementias and Alzheimer’s Disease.
So, for non-caregivers or those who are unfamiliar and inexperienced with these diseases who may be reading this, please don’t assume because you’ve seen or read The Notebook that you’re an expert on the subject and please don’t offer medical diagnoses and advice.
The best gift you can give is to just listen and offer non-medical support. Most caregivers get so deep into the details and all the aspects of these diseases because they need to be able to take care of their loved ones in so many ways that if there were such a thing as a non-M.D. expert on them, most caregivers would qualify.
This post will discuss vascular (multi-infarct) dementia. The cause of this dementia is small vessel ischemia in the brain, which presents itself as chronic transient ischemic attacks (TIA’s). TIA’s are sometimes also referred to as mini-strokes.
TIA’s can occur when the small vessels in the brain get temporarily blocked, cutting off the blood supply and oxygen to that part of the brain. The cumulative affect of these is what causes the damage that is present in vascular dementia. Multi-infarct dementia just means that there are many areas in the brain where this vascular damage has occurred and accrued.
Although high blood pressure is a culprit, high levels of stress and a history of migraines are also players in these kind of TIA’s.
In my mom’s case, all three were factors, but high levels of stress were what brought on the majority of her TIA’s. I suspect she started having these as a small child, because there were times that she just couldn’t remember what happened in a specific instance but she’d referred to it as “blacking out.”
She never lost consciousness with them that I witnessed, but she used the same expression to describes times when we kids were all babies and she was under a lot of stress and she couldn’t remember certain instances of things.
Her TIA’s were common as we grew up, and although we never got over the shock of the suddenness of symptoms and the helplessness we had to do anything about it, we all got pretty good at taking care of her when she had one, and that lasted for Daddy until his death, and for me into adulthood until Mama’s death.
Her TIA’s always presented the same way. They were sudden. Her face would lose all color and her lips would get very pursed as she seemed to salivate more. There was a sort of paralysis except for her right hand. She would start rubbing her thumb across the first two fingers and that would last until the episode was over. I suspect there was a sense of unreality associated with the TIA, so the feeling of her fingers rubbing together was the only reality for her in those episodes.
I’d always hold Mama’s left hand and kind of stroke it so she knew I was there and she wasn’t alone. When the TIA was over, she’d immediately try to talk and everything came out totally garbled. That would last about thirty minutes and then she’d be okay.
And she never remembered them happening. I remember the first time I was giving her medical history as her POA at an ER (and this was way before the dementias and Alzheimer’s Disease) and I named TIA’s as part of her medical history and she disagreed with me and said she didn’t remember ever having those. I laughed at the time and told her that not remembering them was part of the symptom of having them.
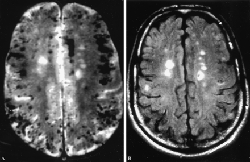 Over time, though, as small vessel ischemia recurs, eventually clusters of damage occur in the brain. This disrupts the normal neurological pathways of how information is learned and communicated. One of the most clear indicators of vascular dementia is difficulty in communication. One of these difficulties is misnaming things.
Over time, though, as small vessel ischemia recurs, eventually clusters of damage occur in the brain. This disrupts the normal neurological pathways of how information is learned and communicated. One of the most clear indicators of vascular dementia is difficulty in communication. One of these difficulties is misnaming things.
For example, the brain knows that a pencil is a pencil. Someone suffering from vascular dementia knows a pencil is a pencil. But because of the damaged pathways, there is often a break in the connection between knowledge and speech, so someone with vascular dementia is just as likely to call a pencil an apple.
Another clear indicator of vascular dementia is slower processing time. A brain with vascular dementia will fight to reroute stored information to speech. However, because of the extensive damage, it has to take a much more convoluted and lengthier route to do that conversion.
A third clear indicator of vascular dementia is that it occurs in sudden, steep steps of decline (brought on by recurrent TIA’s and new clustered areas of damage in the brain). These can occur in a very short period of time, as they did in my mom’s case.
In addition to these definitive indicators, vascular dementia also has features in common with other dementias, including difficulty learning anything new, cognitive impairment, problems with short-term memory, extreme emotional swings, and confusion.
There are no specific treatments for vascular dementia. Unlike any other organ in the body, once the brain has sustained damage, that damage is permanent.
However, there are medications that can address the symptoms of vascular dementia. The two most likely to help are cognitive enhancers: Excelon (although this comes in oral form, the 24-hour patch is best, if there’s no allergic reaction, to get the continual effect of medication that comes in a starting dose of 4.6 mg, a stabilizing dose of 9.5 mg, and a high dose at 13.3 mg) and Namenda (given in 5 mg increments, two to three times a day).
When I discuss the medications in later posts, I will give some practical experience and advice on these two medications, especially with regard to Medicare, the “donut hole,” and working with your loved one’s psychiatrist to get the medication at either no charge or a reduced rate during the “donut hole” period. Both of these are patented, so there’s no cheaper generic version. And paying full price for them will break the bank.
In the next post, we’ll take a look at Lewy Body dementia: what is is, how it’s diagnosed, what it looks like, and effective treatments for the symptoms.
 Winston Churchill had a health profile most of his adult life that pointed to the inevitability of cognitive impairment in his later years.
Winston Churchill had a health profile most of his adult life that pointed to the inevitability of cognitive impairment in his later years. 

