In the fall of 2013, I took the “Care of Elders with Alzheimer’s Disease and Other Major Neurocognitive Disorders” course, which was taught by the John Hopkins School of Nursing. This course is designed for both individual caregivers at home as well as caregivers in a community setting like assisted living facilities and nursing homes.
If you are a caregiver at home for a loved one suffering from dementias and/or Alzheimer’s Disease, I strongly urge you to take this class. It’s free (health professionals can pay a nominal fee to get a certificate and CEU credit for the course) and it’s got a lot of really good information.
Before I talk about the stress effects on our loved ones who suffer with these neurological diseases, let me talk about the course itself. The approach for care being presented by the course is, unfortunately, in my opinion, still largely confined to the halls of academia.
I have never seen the comprehensive – and sensible and workable – and integrated approach to care that is patient-centered this course emphasizes being done in practice in professional (physicians, nurses, hospitals, etc.) and community-based (assisted living and nursing home) environments.
That, in my opinion, is a major shortcoming and flaw in American health care and in the way America treats its elders – as a business commodity off which they make large profits with little effort and little concern, instead of as people who’ve given the best years of their lives to others – their families, their jobs, their country of residence (federal and state taxes, social security, Medicare, etc.) – and who should now be treated with dignity, honor, and respect.
Ironically, though, it is among the individual caregivers of loved ones at home that you see this model that John Hopkins is outlining for care of elders with Alzheimer’s Disease and other major neurocognitive disorders in practice. Not all, but in some.
I certainly know this model was the one I used with my mom. She was the priority. Not me, not anything else, and maintaining her dignity and showing her unconditional love, honor, and respect was paramount. I enforced it with the health care professionals on our team, and those who didn’t or wouldn’t make Mama the priority and treat her with dignity and show her the honor, respect, and love that she deserved were quickly fired by me.
(Most of our team was wonderful, by the way, as individuals; my biggest challenge was always getting and keeping everyone on our team on the same page, and that will always be the biggest challenge for the team leader-caregiver.)
This post will talk about the physiological cycle of stress and the effect of what can become continual stress on our loved ones with dementias and/or Alzheimer’s Disease.
I will also briefly list some of the stressors that our loved ones face. In subsequent posts, I will give some tips and guidelines on how we, as caregivers for our loved ones, can reduce or eliminate some of the stressors that we have control over to alleviate as much as is within our power the sources of stress for our loved ones with dementias and/or Alzheimer’s Disease.
I had to, through observation and trial and error, learn a lot of this on my own with Mama, but because she was my priority, and her comfort, safety, and care along with the continual assurance that she was very much loved were paramount, I took the time (one of three key components missing in a lot of caregiving – the others are patience and slowing down to our loved ones’ paces) to figure it out.
The physiology of stress begins in the brain as a chemical reaction to a demand (real, possible, or perceived) that exceeds a person’s ability to adequately cope.
Stress initiates survival-oriented behavior, which is necessary for surviving acute danger. The neurological response is to turn off the prefrontal brain cortex, which is responsible for intelligent and insightful behavior because we don’t have time to reflect on a course of action in the face of an immediate threat. Instead the “survival centers” in the midbrain take over and cause the brain to react instantly in an instinctive way (the fight-or-flight response associated with lots of adrenaline being released).
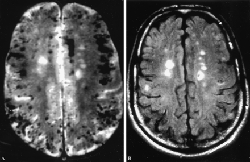
 The picture to the right shows the brain in low and high survival-behavior modes. Note the “holes” in the second image of the picture. These are not actual holes in the prefrontal brain cortex, but are areas which are inactive. That’s about as good a visual of stress’s effect on the brain as you can get.
The picture to the right shows the brain in low and high survival-behavior modes. Note the “holes” in the second image of the picture. These are not actual holes in the prefrontal brain cortex, but are areas which are inactive. That’s about as good a visual of stress’s effect on the brain as you can get.
In every situation where we feel stress, the following reactions occur:
- Cognition is disturbed and can be impaired
- Emotions are disturbed and can be impaired
- Behavior that may adversely affect well-being
An example of cognition being disturbed and impaired is that often in the most intense moment of a stressful situation a condition I’ve always heard referred to as “brain freeze” (inability to think, remember, recall anything for a short period of time) can occur. The brain just locks up. For those of us who are not cognitively-impaired already, that’s a scary situation. Imagine how much more frightening it is for our loved ones who are cognitively-impaired by these diseases.
We have all seen and experienced the intense emotional disturbances and impairments of stress. One example is uncontrollable sobbing. Another is ferocious anger. Like cognition, this emotional disturbance and impairment is even more magnified in our loved ones when they experience stress.
An example of behavior that may adversely affect well-being on the extreme end would be suicide. However, other examples might be throwing things, flinging our bodies against something repeatedly, and self-injury like hitting ourselves or cutting ourselves with a sharp object.
This may seem incomprehensible to someone who’s never had unrelenting and long-term stress so strong that it literally creates an insurmountable and continual deep inner pain that will not go away, but this behavioral aspect seeks to override that internal pain with physical pain, which, in general, is much easier to deal with and is short-lived. However, the results can be devastatingly permanent.
For those of us who are not cognitively-impaired, getting past the action stage of the behavior component is a matter of the ability (and sometimes this is just sheer force of will) to wait it out until it passes (it’s brief, but in times of stress, will recur frequently). For our loved ones suffering from dementias and/or Alzheimer’s disease, many times this ability has either been compromised or lost.
We all know people who do well, most of the time, with a lot of stress and other people who do poorly, most of the time, with even a little bit of stress. Most of how we respond to stress depends on the coping mechanisms we’ve developed over time.
One of the immediate coping mechanisms is the ability to determine whether the stressor is real or perceived. If I see a car going 70 mph heading toward me on a sidewalk, the stress is real. However, if I believe – but don’t know – that something that would negatively impact me could happen, the stress is perceived.
Like my mom, perceived stress is something I – and maybe I’m the only one left now that she’s gone, because it’s not something I hear other people ever talk about – really struggle with and my coping mechanisms are not as good as they should be, although I’m trying to work on improving them.
Mama and I were very different in temperament in some ways, but this is a trait we unfortunately share – Mama because of her experiences, especially during her childhood, and me because I need a plan, need to clearly see the plan, and need to be able to execute the plan, and when periods of life hit where there’s no visible plan and I’m in what feels like interminable limbo hell, I get stressed to the max.
A lifetime of chronically high stress levels combined with poor coping mechanisms is now being linked, by scientific research, to a risk of developing vascular dementia (the result of strokes and TIA’s) and Alzheimer’s Disease. One of the responders to stress is a hormone produced by the adrenal gland called glucocorticoids. Repeated exposure to glucocorticoids accelerates the aging process of the brain and damages and shrinks brain tissue, which is clearly seen in Alzheimer’s disease.
 This gives me more incentive to quickly and drastically improve my coping mechanisms (and I admit, so far, I’m failing way more than I’m succeeding, but I’m determined to make this happen) because I know that Mama’s poor coping mechanisms to stress played a role – not the only one – in her development of vascular dementia and Alzheimer’s Disease.
This gives me more incentive to quickly and drastically improve my coping mechanisms (and I admit, so far, I’m failing way more than I’m succeeding, but I’m determined to make this happen) because I know that Mama’s poor coping mechanisms to stress played a role – not the only one – in her development of vascular dementia and Alzheimer’s Disease.
As our loved ones become more cognitively-impaired by these diseases, more and more things of everyday life become stressors (real or perceived) and their anxiety-tolerance thresholds get lower and lower, until almost anything can be a source of stress.
Since we know one of the results of stress is cognitive disturbance and impairment, stressors for our loved ones with dementias and/or Alzheimer’s Disease create even greater cognitive disturbance and impairment, in the form of more confusion, more agitation, more anxiety, more restlessness. There can be a serious and sudden decline in cognitive function because of a stressor that we may or may not be aware of. In addition, we see the emotional and behavioral disturbances and impairments in exaggerated form as well (crying, yelling, hitting, biting, and pacing are common emotional and behavioral manifestations).
However, a lot of these stressors are easily remedied or eliminated, which we will discuss in the next few posts on this topic. For now, though, I’ll list of some of the most common stressors that we’ll be looking at:
- Unmet needs
- Physical environments
- Routines
- Communication
- Hearing
- Vision
- General physical health
We’ll begin next week looking at these specifically to see how they can be stressors and what we, as loving caregivers, can do to remedy or eliminate them as stressors for our loved ones.